Surgical Procedures
Apical Surgery
If a root canal treated tooth has a new or persistent infection and it does not seem that retreatment will address the problem, then apical surgery may be required. Fortunately, apical surgery is required less than 5-10% of the time after a root canal but in general, the larger the infection was to start, or the longer it had been present, the higher the chance of the infection not healing. Apical surgery involves making an incision in the gum line and accessing the infected area directly through the side of the bone. The infected tissue and a small portion of the tip of the root are removed to allow a filling (special calcium cement material) to be placed into the root tip and seal the root. Sutures are placed and typically removed after 5-7 days.
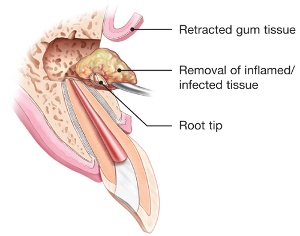
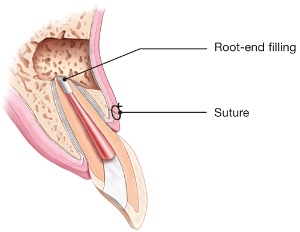
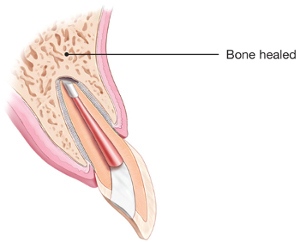
Intentional Replantation
Occasionally, there can be a situation where retreatment will not work predictably to address an infection, but the tooth is located in an area where direct surgical access is very difficult or impossible. Intentional replantation may be the only last option to retain a tooth in this situation, but prognosis depends on individual circumstances of each case. During this procedure, the tooth is extracted and the apical surgery is performed with the tooth in hand. Then the tooth is placed back into the tooth socket. Depending on the stability of the replanted tooth, a small piece of wire may be used to splint to tooth in place. If the tooth is outside the mouth for a minimal amount of time, then the ligament cells coating the root surface will typically stay alive and heal by reforming the tooth ligament after replantation. It is the same goal as when a child knocks a tooth out and it is kept in milk or saline solution and replanted quickly, a majority of the time the ligament and bone will heal and the tooth can be retained. The main risk with replantation is that the ligament does not heal normally and resorption of the root or persistent infection occurs. The other risk of intentional replantation is that the tooth cracks during the extraction and cannot be replanted. If there are no other viable options to retain a tooth and replantation seems possible, we will discuss prognosis and treatment alternatives to help you decide what treatment is best for you. Intentional replantation may not be as predictable as other endodontic procedures so if prognosis seems too questionable, then extraction and either an implant or bridge may be indicated.
Extraction and Bone Grafting
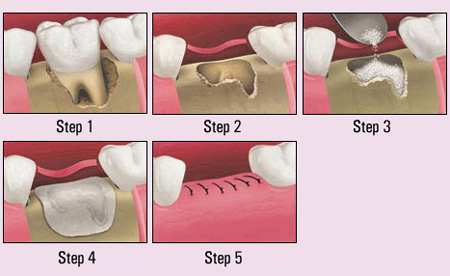 If a tooth is cracked or has a poor prognosis for any other reason, then extraction and tooth replacement with an implant or bridge may be required. If an implant is planned, then grafting the tooth socket at the time of extraction is usually indicated to help regrow and maintain the maximum amount of jaw bone for implant stability. If an implant is definitely not going to be placed, then the graft may not be necessary and just the extraction may be all that is required. Dr. Palte does not place implants, but he will occasionally perform extractions and can place bone grafts if necessary. This is usually in circumstances where the patient is already numb and the fracture or problem was found during attempted root canal treatment or apical surgery. If the poor prognosis is discovered during the examination, then your general dentist will be consulted to determine the best course of action. Evaluation of the area by an implant specialist may be beneficial before the tooth is extracted, so you may be referred to the implant surgeon for treatment.
If a tooth is cracked or has a poor prognosis for any other reason, then extraction and tooth replacement with an implant or bridge may be required. If an implant is planned, then grafting the tooth socket at the time of extraction is usually indicated to help regrow and maintain the maximum amount of jaw bone for implant stability. If an implant is definitely not going to be placed, then the graft may not be necessary and just the extraction may be all that is required. Dr. Palte does not place implants, but he will occasionally perform extractions and can place bone grafts if necessary. This is usually in circumstances where the patient is already numb and the fracture or problem was found during attempted root canal treatment or apical surgery. If the poor prognosis is discovered during the examination, then your general dentist will be consulted to determine the best course of action. Evaluation of the area by an implant specialist may be beneficial before the tooth is extracted, so you may be referred to the implant surgeon for treatment.
